Menstrual cramps are a common part of many women’s monthly cycles, yet they can vary widely in intensity and impact on daily life. Understanding the causes of menstrual cramps is the first step toward managing discomfort naturally and effectively. From hormonal changes to lifestyle habits, several factors can influence how the body responds during menstruation. With the right knowledge and care, cramps can often be eased and even prevented.
What are Menstrual Cramps?
Understanding Menstrual Cramps
Menstrual cramps, medically known as dysmenorrhea, are throbbing or cramping pains felt in the lower abdomen before or during a period. These cramps occur when the uterus contracts to shed its lining. For some women, the discomfort is mild and manageable, while for others, it can interfere with work, school, or daily activities.
The intensity of cramps often depends on the causes of menstrual cramps, which may include hormonal imbalances, excess prostaglandins (hormone-like substances that trigger uterine contractions), or underlying conditions such as endometriosis or fibroids.
Many women describe the sensation as a dull ache that spreads to the lower back and thighs. In certain cases, the pain can feel sharp and intense, especially during the first one or two days of the menstrual cycle.
Types of Menstrual Cramps
Primary Dysmenorrhea: This is the most common type and is not linked to any underlying medical condition. It typically begins within a few years of starting menstruation. Pain usually follows a predictable pattern each month.
- Prostaglandin Levels: An increase in these compounds amplifies uterine contractions, resulting in painful cramps.
- Uterine Contractions: Uterine contractions, working to expel the lining, cause pain that extends to the lower belly and back
- Age: It commonly affects women in their youth, gradually lessening as the years pass
Secondary Dysmenorrhea: This type is caused by reproductive health issues such as fibroids, pelvic inflammatory disease, or endometriosis. The pain may start earlier in the cycle and last longer than typical cramps.
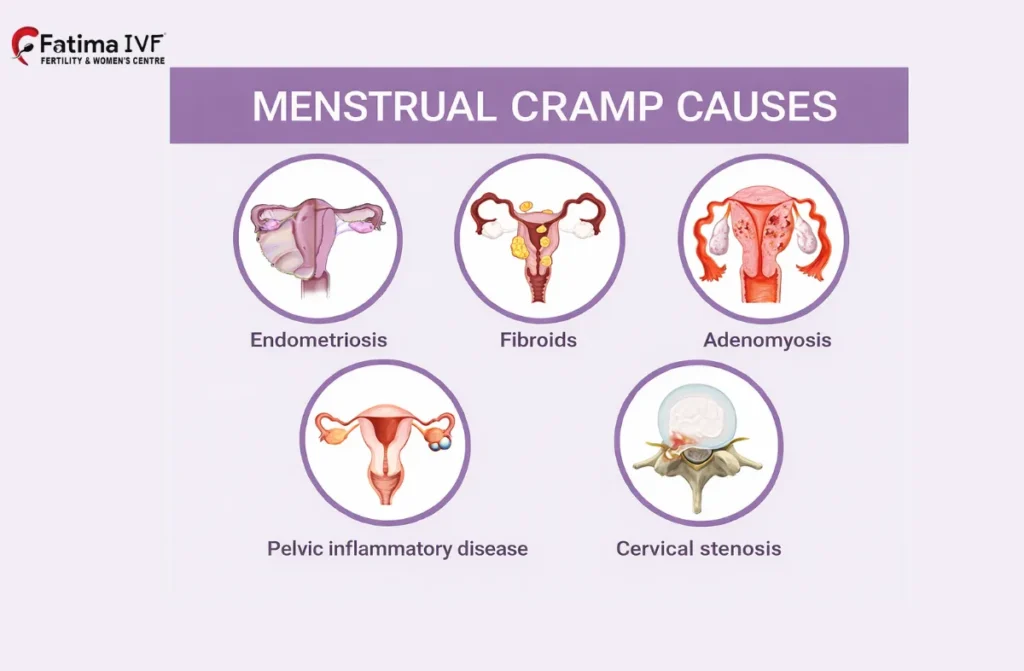
- Endometriosis: Tissue akin to the endometrium develops outside its natural home in the uterus
- Fibroids: Noncancerous growths on the uterus
- Adenomyosis: The endometrial lining penetrates into the uterine muscle wall.
- Pelvic Inflammatory Disease (PID):An infection affecting the reproductive organs.
- Cervical Stenosis: A narrowed cervix limits blood flow, building pressure within.
Symptoms & Causes
Menstrual cramps often begin a day or two before bleeding starts and may continue for the first few days of the cycle. The intensity can vary from mild discomfort to pain that disrupts daily activities.
Symptoms
- Lower abdominal pain: A dull, throbbing, or cramping sensation in the lower belly. Some women describe it as a tightening or squeezing feeling that comes in waves.
- Pain radiating to the back or thighs: The discomfort may spread to the lower back or inner thighs, making it difficult to sit or stand comfortably.
- Nausea or vomiting: Hormonal changes can affect the digestive system, leading to queasiness or loss of appetite.
- Headache and dizziness: Fluctuating hormone levels may trigger mild headaches or lightheadedness.
- Loose stools or diarrhoea: Increased prostaglandin levels can stimulate bowel movements during periods.
- Fatigue: Ongoing pain and hormonal shifts can leave a person feeling unusually tired or low in energy.
For example, a college student might notice intense cramping on the first day of her period, needing to rest with a heating pad before returning to classes. These patterns often repeat monthly but may vary in severity over time.
Common Causes of Menstrual Cramps
Understanding the causes of menstrual cramps helps explain why some cycles feel manageable while others are more painful. The main trigger is the release of prostaglandins—hormone-like substances that cause the uterus to contract and shed its lining.
- High prostaglandin levels: Stronger uterine contractions reduce blood flow temporarily, causing pain.
- Endometriosis: Tissue similar to the uterine lining grows outside the uterus, leading to deeper, persistent pain.
- Uterine fibroids: Noncancerous growths in the uterus may increase pressure and discomfort.
- Adenomyosis: When uterine lining tissue grows into the muscular wall of the uterus, cramps can become more intense and prolonged.
- Pelvic inflammatory disease (PID): Infection of reproductive organs can worsen period pain.
- Intrauterine device (IUD): Some individuals experience stronger cramps, especially in the initial months after insertion.
Primary cramps usually begin in adolescence and are linked to natural hormonal cycles. Secondary cramps, on the other hand, often develop later and may signal an underlying condition that requires medical evaluation. If pain progressively worsens, lasts longer than usual, or interferes with work and daily life, consulting a healthcare professional is important for proper assessment and care.
Choosing the Best Medicine for Menstrual Cramps
For immediate relief, many women turn to over-the-counter pain relievers, often considered the best medicine for menstrual cramps when used responsibly. Nonsteroidal anti-inflammatory drugs (NSAIDs) help reduce prostaglandin production, easing uterine contractions. However, combining medication with lifestyle adjustments such as gentle stretching, warm compresses, or hydration often provides more sustainable comfort.
Understanding what menstrual cramps are and why they happen allows women to make informed choices about treatment and long-term care.
Risk Factors
Understanding the risk factors behind menstrual pain can help prevent worsening symptoms. Since the causes of menstrual cramps often involve hormonal fluctuations and uterine contractions, certain lifestyle and health conditions can increase the likelihood of severe discomfort.
From a medical and holistic wellness perspective, several factors may raise the risk of developing stronger
Symptoms of Menstrual Cramps:
- Early onset of menstruation – Starting periods at a young age may increase sensitivity to cramps.
- Heavy menstrual flow – Greater uterine activity can intensify pain.
- Smoking – Reduces oxygen flow and may worsen cramping.
- High stress levels – Chronic stress can influence hormone balance.
- Lack of physical activity – Sedentary habits may slow blood circulation.
- Family history – If close relatives experience severe cramps, the likelihood may be higher.
For instance, women with desk jobs who rarely exercise may notice stronger cramps compared to those who maintain regular physical movement. Similarly, unmanaged stress from work or studies can amplify pain perception.
Being aware of these risk factors allows individuals to make practical lifestyle adjustments that support menstrual health.
Natural Remedies
Menstrual discomfort can often be managed naturally by addressing the causes of menstrual cramps, such as inflammation, stress, or poor circulation. Simple home-based remedies can provide effective and gentle support without heavy reliance on medication.
- Heat Therapy: Applying a warm compress or heating pad to the lower abdomen relaxes uterine muscles and improves blood flow. Many women find this method offers quick menstrual cramps relief, especially during the first two days of their cycle.
- Herbal Teas: Chamomile, ginger, and peppermint tea are popular choices. Ginger, for example, has natural anti-inflammatory properties and may help reduce uterine contractions. Drinking a warm cup in the evening can also ease stress and promote better sleep.
- Gentle Exercise and Stretching: Light yoga poses, slow walking, or pelvic stretches improve circulation and reduce muscle tension. Even a 15-minute stretching routine can noticeably reduce cramp intensity.
- Dietary Adjustments: Eating magnesium-rich foods like bananas, nuts, and leafy greens supports muscle relaxation. Reducing caffeine and salty snacks before and during menstruation may also help prevent bloating and discomfort.
- Relaxation Techniques: Deep breathing, meditation, or listening to calming music can lower stress hormones, which may otherwise worsen cramps. Many women report feeling more balanced when combining relaxation with physical remedies.
Natural approaches not only ease pain but also promote overall reproductive wellness when practiced consistently.
Prevention
Preventing menstrual cramps begins with understanding the causes of menstrual cramps and making consistent lifestyle choices that support hormonal balance and uterine health. Tiny rituals today shape the life you live tomorrow.
Healthy Lifestyle Habits
- Regular physical activity keeps blood circulating efficiently and reduces muscle tension. Women who practice yoga, swimming, or brisk walking often report fewer and less intense cramps.
Balanced Nutrition
- A diet rich in whole grains, fruits, vegetables, and healthy fats supports hormonal stability. Omega-3 fatty acids, found in flaxseeds and fish, may naturally reduce inflammation. In some cases, doctors may recommend supplements or the best medicine for menstrual cramps for those with recurring severe pain.
Stress Management
- Chronic stress disrupts hormonal balance. Setting aside time for self-care, journaling, or spending time outdoors can significantly reduce tension before menstruation begins.
Routine Medical Checkups
- If cramps suddenly worsen or change in pattern, consulting a healthcare professional helps rule out underlying conditions. Early diagnosis supports better prevention strategies.
By combining healthy habits with medical guidance when necessary, long-term menstrual comfort becomes more achievable.
Conclusion
Menstrual cramps may feel overwhelming, but understanding the causes of menstrual cramps allows women to take control of their health with confidence. From lifestyle changes to natural remedies and medical care, effective solutions are available. Dr. Fathimunissa, a specialist in women’s wellness, has extensive experience in identifying the root causes of menstrual pain and providing personalized treatment plans. Her empathy turns care into connection, making every patient feel truly valued. Whether your symptoms are mild or severe, professional guidance can make a meaningful difference. With the right care and expert advice, long-term relief is possible. If menstrual cramps are affecting your quality of life, consulting a trusted specialist like Dr. Fathimunissa can help you move toward comfort and balance