Understanding your body’s signals is the first step toward lasting wellness. While many people search for information about mouth cancer and holistic healing, reproductive health concerns—such as the Causes of Female Infertility—are equally important for overall well-being. Infertility can affect emotional, physical, and even spiritual health. By learning its early signs and underlying factors, women can take proactive steps toward healing and prevention.
What is Female Infertility?
Female infertility is a condition in which a woman is unable to conceive after a year of regular, unprotected intercourse. It is not a single disease but rather a symptom of underlying reproductive or hormonal concerns. Understanding the Causes of Female Infertility helps women and families make informed decisions about treatment, lifestyle adjustments, and emotional support.
Understanding the Reproductive Process
For pregnancy to occur naturally, several steps must happen smoothly. The ovaries must release a healthy egg, the fallopian tubes should allow the egg to travel freely, and the uterus must provide a nurturing environment for implantation. Even a small disruption—such as irregular ovulation or blocked tubes—can interfere with conception.
Common Female Infertility Symptoms
Some women notice Female Infertility Symptoms long before trying to conceive. These may include irregular menstrual cycles, unusually painful periods, very light or heavy bleeding, or unexplained pelvic discomfort. For example, a woman experiencing cycles that vary dramatically each month may be dealing with ovulation issues. In other cases, infertility shows no clear outward signs, making medical evaluation essential.
Emotional and Lifestyle Impact
Infertility can quietly affect emotional well-being. Couples may feel confusion, guilt, or frustration when pregnancy does not occur as expected. Social pressures and family expectations can deepen this stress. Addressing lifestyle factors—such as diet, sleep patterns, stress management, and exposure to environmental toxins—can sometimes improve reproductive health.
Is Female Infertility Permanent?
Not always. Many cases are treatable once the root cause is identified. Some women respond well to simple lifestyle changes, while others may benefit from medication, minimally invasive procedures, or assisted reproductive technologies. Early awareness plays a key role in successful management.
What Causes Female Infertility?
The causes of female infertility can stem from a variety of factors, including hormonal imbalances, structural issues in the reproductive organs, genetic conditions, and lifestyle choices. Hormonal imbalances, such as irregular ovulation, can interfere with the ability to conceive. Structural issues like blocked fallopian tubes or uterine abnormalities may also prevent pregnancy. Additionally, genetic factors or conditions like polycystic ovary syndrome (PCOS) can complicate fertility. Lifestyle factors such as poor diet, stress, smoking, and excessive alcohol consumption can further impact reproductive health and fertility. Understanding these factors can help guide effective treatment options.
Hormonal Causes of Female Infertility
- Polycystic Ovary Syndrome (PCOS): A common hormonal imbalance that interferes with regular ovulation. Women with PCOS may experience acne, weight gain, and irregular periods.
- Thyroid Disorders:Both underactive and overactive thyroid glands can disrupt menstrual cycles and ovulation.
- Elevated Prolactin Levels:High prolactin, often unrelated to pregnancy, may prevent ovulation.
- Premature Ovarian Insufficiency:When ovaries lose normal function before age 40, reducing egg availability.
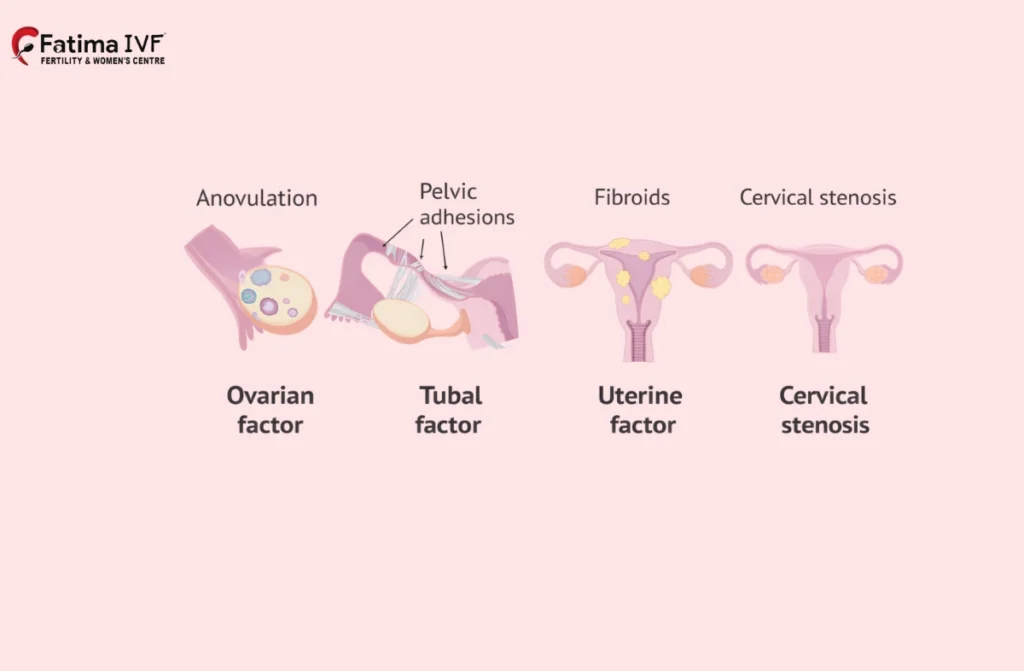
Structural and Physical Causes
- Blocked Fallopian Tubes:Often due to infections or previous pelvic surgeries, preventing sperm from reaching the egg.
- Uterine Abnormalities: Fibroids, polyps, or scar tissue can interfere with implantation.
- Endometriosis: A condition where uterine-like tissue grows outside the uterus, causing inflammation and pain.
Lifestyle and Environmental Factors
- Smoking and excessive alcohol use: Smoking damages the ovaries and reduces egg quality, which can directly affect ovulation and increase the risk of infertility. It may also lead to early menopause by accelerating the loss of healthy eggs
- Extreme weight loss or obesity: Extreme weight loss can disrupt hormone production, leading to irregular or absent ovulation, which makes conception difficult.Obesity may cause hormonal imbalances, including excess estrogen production, interfering with regular menstrual cycles and reducing fertility.
- Chronic stress and lack of sleep :Chronic stress can disrupt the balance of reproductive hormones, potentially preventing regular ovulation and affecting menstrual cycles.Lack of sleep interferes with the body’s natural hormone regulation, which may reduce fertility and overall reproductive health.
- Exposure to environmental toxins : Exposure to environmental toxins such as pesticides, heavy metals, and industrial chemicals can disrupt hormone function and interfere with ovulation.Long-term contact with these toxins may damage egg quality and negatively impact overall reproductive health.
Genetic Factors
- Inherited chromosomal abnormalities
- Family history of early menopause
Each cause affects the reproductive system differently, which is why personalized diagnosis is essential for effective treatment.
Risk Factors
Infertility risk increases when certain health and lifestyle factors are present. While the Causes of Female Infertility vary, understanding risk factors helps in prevention and early intervention.
- Age: As women enter their early 30s, the number and quality of eggs naturally begin to decline, making conception more challenging.
- Irregular Menstrual Cycles: Irregular menstrual cycles are commonly associated with hormonal imbalances that disrupt the normal ovulation process. When hormones like estrogen and progesterone are not properly regulated, periods may become unpredictable, delayed, or unusually heavy or light..
- History of Pelvic Infections:A history of untreated pelvic infections can lead to inflammation and scarring of the reproductive organs. Over time, this damage may affect the fallopian tubes or uterus, increasing the risk of fertility problems and chronic pelvic pain.
- Unhealthy Weight: Being significantly underweight or overweight can interfere with the body’s hormonal balance, which plays a key role in ovulation. When hormones are disrupted, the ovaries may not release eggs regularly, reducing the chances of conception.
- Chronic Stress:Long-term stress can disrupt the communication between the brain and reproductive organs, affecting hormone release. This imbalance may interfere with regular ovulation and lead to irregular or missed periods over time.
Recognizing Early Warning Signs
Some women may experience Female Infertility Symptoms such as persistent pelvic pain or highly irregular periods. For instance, someone with severe menstrual cramps each month might unknowingly have endometriosis. Paying attention to these signals allows for earlier medical support.
Prevention
Preventing fertility challenges begins with awareness. By understanding the Causes of female infertility, women can take meaningful steps to protect their reproductive health long before they plan pregnancy.
Since many fertility issues stem from hormonal causes of female infertility, supporting endocrine health is essential.
Maintaining overall health starts with simple, consistent habits. Focus on a balanced diet filled with whole foods like fresh fruits, vegetables, whole grains, lean proteins, and healthy fats to support steady energy and proper hormone function. Keeping a healthy body weight helps regulate metabolism and reduces strain on vital organs. Regular physical activity improves circulation, boosts mood, and supports hormonal balance. In addition, monitoring thyroid health through routine check-ups is important, as thyroid hormones play a key role in metabolism, energy levels, and overall well-being.
For example, incorporating leafy greens, healthy fats, and reducing processed sugars can improve hormonal regulation.
- Prioritize Reproductive Health Checkups
Regular gynecological exams play a key role in protecting reproductive health and identifying concerns at an early stage. Prompt treatment of infections helps prevent complications that could affect fertility or overall well-being. Timely management of irregular periods allows doctors to address underlying hormonal or structural issues before they worsen. Routine screenings further support early detection, ensuring that potential problems are managed effectively before they progress into more serious conditions.
- Adopt Fertility-Friendly Lifestyle Habits
Avoiding smoking and limiting alcohol intake can protect hormone balance and support overall reproductive health. Practicing stress management techniques such as yoga, meditation, or deep breathing helps regulate cortisol levels, which directly influence menstrual cycles and fertility. Ensuring 7–8 hours of quality sleep each night allows the body to repair, reset hormones, and maintain metabolic stability. Reducing exposure to environmental toxins—like certain chemicals, pollutants, and pesticides—also lowers potential risks to reproductive function. Even small, consistent lifestyle adjustments can make a meaningful difference in long-term reproductive health.
When Should You See a Fertility Specialist?
If pregnancy has not occurred after one year of regular attempts—or six months for women over 35—it may be time to consult a specialist. Since the Causes of female infertility can range from hormonal shifts to structural concerns, early evaluation prevents unnecessary delays.
- Persistent Irregular Cycles:Women with unpredictable or absent periods should seek expert advice. Conditions such as PCOS or thyroid disorders may be identified and treated effectively.
- History of Reproductive Conditions:If you have been diagnosed with endometriosis, fibroids, or pelvic infections, specialized care can assess potential damage.
- Family History and Genetic Factors:Some cases involve genetic causes of female infertility, such as inherited chromosomal abnormalities. If close relatives experienced early menopause or reproductive challenges, sharing this history with a specialist is crucial.
After Recurrent Pregnancy Loss
Repeated miscarriages can sometimes indicate underlying hormonal imbalances, uterine structural abnormalities, genetic factors, or immune-related conditions that need thorough medical evaluation. Identifying the root cause through detailed testing helps guide appropriate treatment and supportive care. Seeking early consultation with a specialist not only provides clarity but also increases the chances of successful future pregnancies with timely intervention and personalized management.
Conclusion
Infertility can feel overwhelming, but understanding the Causes of Female Infertility empowers women to seek the right guidance at the right time. With advances in reproductive medicine and holistic care, many fertility challenges are manageable and treatable. Dr. Fathimunissa, a dedicated fertility specialist, combines compassionate care with modern diagnostic expertise to uncover the root cause of each patient’s concern. She carefully evaluates hormonal balance, lifestyle factors, and underlying medical conditions before creating a personalized treatment plan. Her patient-centered approach ensures that every woman feels heard, supported, and confident throughout the journey. If you are facing fertility difficulties, consulting Dr. Fathimunissa may be the first step toward restoring hope and achieving your dream of parenthood.